
NHS Implant Eligibility & Cost Estimator
Your Situation
Answer honestly to get an accurate assessment of your funding pathway.
Analysis Results
Fill out the checklist to see your options.
You’ve heard the rumors. You’ve seen the online forums buzzing about people walking away from a dental surgery in London or Manchester with brand new teeth and zero bills. The question on everyone’s mind is simple but loaded with anxiety: who qualifies for free dental implants UK? If you are struggling to find an answer, you’re not alone. We all want affordable smiles, but the reality of the British healthcare system can feel like navigating a maze in the dark.
The short answer is going to disappoint most readers, but the long answer provides a path forward. True "free" dental implants through the National Health Service (NHS) are exceptionally rare. For the vast majority of citizens, getting an implant means paying privately. However, there are specific, narrow exceptions where the state will cover these procedures. Understanding these distinctions is crucial because chasing a free procedure when it isn't available to you wastes months of your life.
The NHS Dental System Explained
To understand why dental implants aren’t standard issue, you have to look at how the NHS prioritizes care. The National Health Service, which runs public healthcare across the United Kingdom, operates on a foundation of treating illness and pain before aesthetics. NHS Dentistry classifies treatments into three bands based on complexity and duration. Band 1 covers basic exams and cleaning. Band 2 includes fillings and extractions. Band 3 is for major work like crowns and dentures. While a standard tooth extraction falls into Band 2, replacing that missing tooth with an implant usually sits outside these bands entirely. In the UK, denture plates and fixed bridges are considered more cost-effective solutions for replacing missing teeth compared to surgical implants. Therefore, under routine General Dental Services (GDS), a local GP won’t be able to give you an implant for free. The logic follows a strict hierarchy of clinical need versus financial impact.
When Will the NHS Actually Pay?
If a dentist tells you the NHS will never touch your case, ask them to clarify their reasoning. While GDS (your regular high-street dentist) rarely offers them, there is another tier called Specialist Dental Services. This tier handles complex cases where a patient genuinely cannot survive without the procedure.
- Cancer Reconstruction: Patients undergoing treatment for oral cancer may need implants placed to anchor prosthetics after jaw removal surgery. In these scenarios, the NHS often funds the full reconstruction as part of the oncology pathway.
- Trauma Cases: If you lose multiple teeth due to a car accident or violence, and the damage is extensive enough to require bone grafting or maxillofacial surgery, the hospital service may step in to manage the rehabilitation.
- Congenital Defects: Children born with cleft palates or severe developmental issues often fall under specialized orthodontic programs where implant-supported prosthetics might be provided at no cost.
This distinction matters because many people confuse "missing teeth" with "medical necessity." Just because a tooth causes embarrassment doesn’t make it a medical emergency in the eyes of the state. However, if the lack of teeth affects your ability to eat, breathe, or maintain airway safety, the argument shifts toward clinical necessity.
Hospital vs. High Street: The Referral Battle
Your route to potential coverage depends heavily on whether you see a Community Dental Officer (CDO) or go straight to a university clinic. The journey starts with a referral from your local GP or a high-street dentist who confirms you do not qualify for General Dental Services.
In England, Scotland, Wales, and Northern Ireland, rules vary slightly regarding funding allocation. In England, the Integrated Care Boards (ICBs) review individual cases where someone claims they need a hospital-based solution. These reviews are rigorous. They scrutinize whether less invasive options (like partial plates) were offered and refused by the patient for non-medical reasons.
Let's say you have no back molars. A dentist suggests bridges. You refuse them because they are too tight. The hospital system will likely deny you because a bridge is a valid, cheaper alternative that restores function. You win points for an appeal if you can prove that alternatives simply cannot work physically-such as lacking bone density to anchor a bridge abutment.
| Patient Condition | Likelihood of Coverage | NHS Pathway |
|---|---|---|
| Standard Tooth Loss | Very Low | Excluded; usually treated with dentures. |
| Post-Cancer Surgery | High | Oncology Department / Special Needs Clinic. |
| Maxillary Fracture | Moderate | Oral & Maxillofacial Unit referral. |
| Blood Disorders (Factor VIII) | Moderate | Requires specialist hospital management. |
The Unseen Option: University Dental Schools
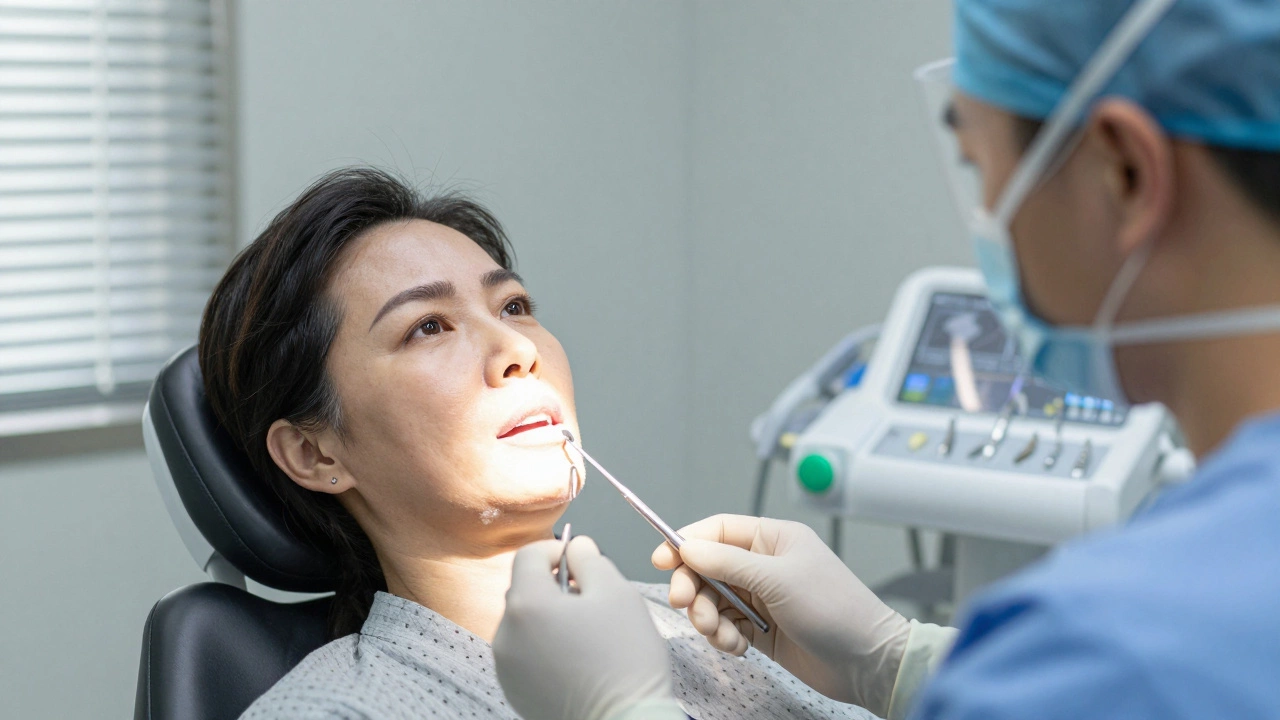
If the NHS door slams shut, your next best bet involves academic institutions. Major teaching hospitals in cities like Bristol, Manchester, Newcastle, and Cardiff host dental schools. These facilities operate clinics where final-year students perform procedures under strict supervision by senior clinicians.
This setup creates a unique environment where treatments are significantly cheaper than private practices, sometimes bordering on free depending on your income bracket. It isn't officially "free" in the sense of zero cost, but the fees are capped at subsidized rates set by the educational board rather than commercial pricing.
The trade-off? Time. You will be treated by a student. While the oversight is intense and safety protocols are ironclad, appointments take longer. One session at a private practice might last 90 minutes; at the university clinic, that same session could stretch over two weeks of visits. If you have patience and budget constraints, this is arguably the closest mechanism to getting near-free access in the UK today.
Charity Work and Financial Hardship Funds
Does a national "charity" exist that simply hands out cash for teeth? Not exactly. However, organizations focusing on health inequalities play a vital role. There are local groups, such as the East London Foundation Trust or various community health hubs, that occasionally fundraise for patients facing homelessness or extreme poverty.
These are not guaranteed routes. You would typically need to be referred by a social worker or housing officer. Furthermore, some dental manufacturers offer discount schemes. Companies that produce the hardware for implants sometimes subsidize clinics to gain placement data or testing rights. While you rarely walk away completely debt-free, these programs can knock thousands off the final tab.
It also pays to look into credit union loans specifically tailored for health. Many UK residents turn to interest-free loans offered by credit unions, distinct from predatory payday lenders. While not technically "free," spreading the cost without interest makes the burden manageable, essentially functioning as a form of financial aid.
Social Prescribing and Mental Health
A relatively modern shift in UK healthcare strategy involves "Social Prescribing." If your dental decay is linked to mental health struggles-perhaps an addiction leading to neglect or severe depression preventing self-care-you might qualify for wrap-around support.
This pathway links your primary care provider with community organizations. Sometimes, these organizations have partnerships with sympathetic local surgeries that agree to reduced rates for vulnerable populations. It’s an indirect method of accessing free care, relying on broader public health goals rather than pure dental funding.
Imagine a scenario where you are unemployed, homeless, and suffering from untreated gum disease. A link worker connects you to a project funded by the Public Health Grant. That grant covers hygiene education and potentially advanced restorative work if deemed necessary for systemic health recovery. It's niche, but it does exist.
Preparing for Private Funding
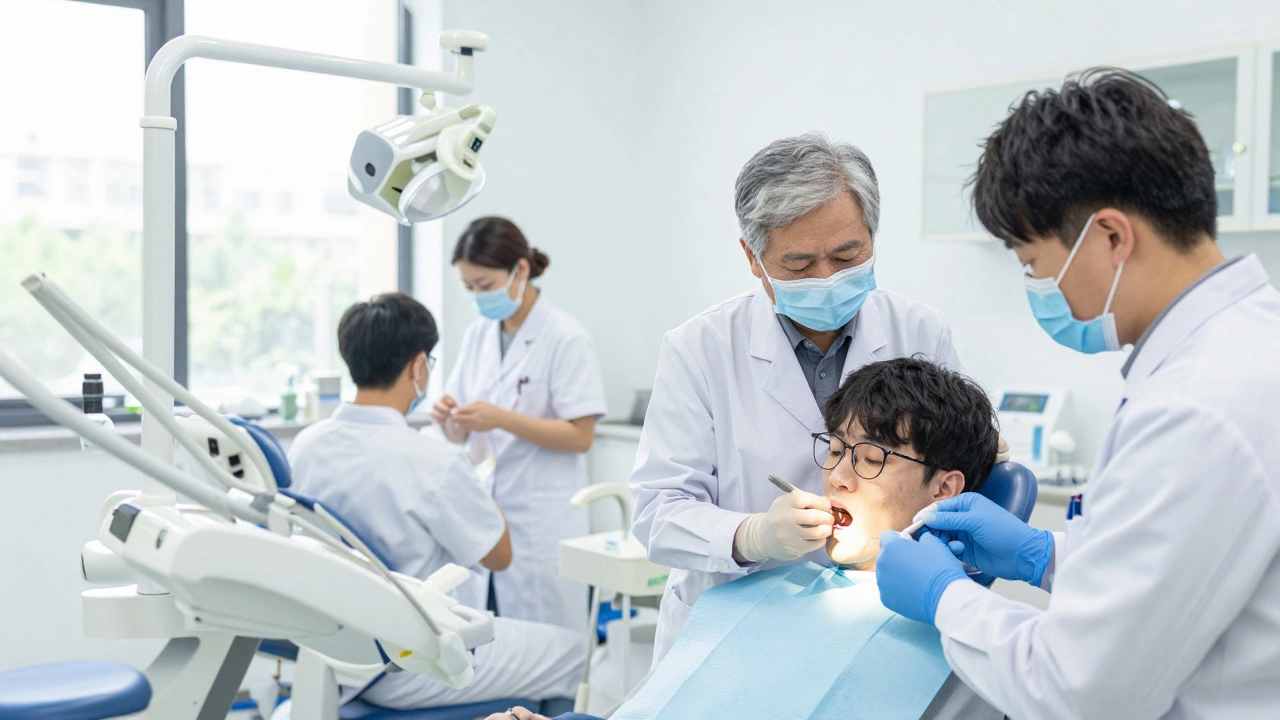
Let’s be realistic about the odds. Unless you fit the very strict NHS medical criteria discussed earlier, private funding is the expected route. The UK has robust consumer protections here. Before signing up for a £20,000 plan, verify that the clinic uses implant brands like Straumann or Nobel Biocare which come with 10-year warranties.
Most reputable clinics now offer interest-free payment plans up to 36 months. Spreading $12,000 over three years makes monthly payments look like car insurance premiums. Additionally, some companies specializing in dental equipment offer financing directly to patients through third-party partners. Always read the terms-some "free interest" deals balloon in total value once administrative fees hit.
Regional Nuances: Where You Live Matters
We must acknowledge that the UK is not one uniform block. Funding discretion rests with regional bodies known as Clinical Commissioning Groups (CCGs) or Health Boards in Scotland and Wales. A case approved in Greater Manchester might be rejected in Cornwall purely because different committees interpret "clinical need" differently.
If you are willing to move temporarily for treatment, checking policies in neighboring counties can yield results. Some regions have aggressive "Dental Voucher" schemes for low-income adults that include a clause allowing for implants if a bridge fails. These vouchers are often limited quantities and require application well before the actual treatment date.
The Bottom Line on Costs
To manage expectations, knowing the baseline prices helps avoid shock. A single upper anterior implant in a private London clinic might run you £3,000 to £4,500 including the crown. Bone grafting adds another £800 to £1,200. The NHS equivalent-a removable partial denture-is usually around £1,200 maximum depending on the band fee.
Compare that cost-benefit analysis with the likelihood of rejection for NHS implants. Most patients end up choosing a hybrid approach: NHS dentures initially, saving money, then upgrading to a private implant later when finances improve. It’s not immediate gratification, but it is a strategy used by thousands across the country.
Can you get NHS dental implants on the basis of age?
No. Age alone does not qualify you for NHS dental implants. Even if you are elderly, the NHS typically provides dentures as a standard replacement for missing teeth unless there is a complex medical reason requiring an implant specifically.
Is there any way to apply for free dental implants through the government?
There is no central government grant specifically for cosmetic dental implants. However, if you face severe hardship, you may apply for a Patient Group Direction waiver or seek help through specific charity trusts managed by local councils, though approval rates are extremely low.
Do dental schools offer free implants to the public?
Some university dental hospitals offer subsidized rates that are significantly lower than private fees. They rarely provide services for absolutely free, but they do accept NHS patients in some circumstances if no other treatment option is viable.
Will the NHS cover implants if I had an accident?
Traumatic injury resulting in tooth loss may be eligible for specialist hospital care. If your mouth was severely damaged by violence or a vehicle collision, an Oral Surgeon assessment is required to determine if implants are necessary for functional repair.
Are there tax credits for dental work in the UK?
No, medical expenses for dental work cannot be claimed back through tax credits or HMRC unless you have specific disability-related benefits that might cover equipment rental, not permanent fixtures.